Inside Burkina Faso’s Mosquito Dome, Where Venomous Fungus Is Put to the Test
An innovative research center dedicated to blood, biting, and beating back malaria.

Somewhere off the main road in the village of Soumousso in Burkina Faso is another village—built entirely for mosquitoes. It doesn’t look quite like the others in the southwest of the country, or anywhere else, for that matter. There are a few huts, but they reside within domes of fine mesh netting that cover an area approximately the size of three tennis courts. In the place of beds, there are small pools of stagnant water. And there are no human residents, just several calves who are well-fed and blithely unaware that they have been offered up as a smorgasbord for the world’s most annoying bug. But it takes a village to raise (and kill) a mosquito.
This quasi-village is the brainchild of researchers from the United States and Burkina Faso, who call it the MosquitoSphere. For several years, they’ve been using it as a lab to test the latest weapon in the country’s ongoing battle with malaria: a transgenic fungus biologically engineered with spider venom to put mosquitoes—and the pathogens they carry—in an early grave. And it seems to have worked, with 99 percent of the mosquitoes trapped with the fungus dying within a month of testing. The researchers, from the University of Maryland and the Research Institute of Health Sciences & Centre Muraz in Bobo-Dioulasso, Burkina Faso, recently published their results in the journal Science.
Burkina Faso is one of the worst places in the world to be bitten by a mosquito, which helps make it one of the best places in the world to study malaria. With more than 7.9 million cases of the parasitic disease recorded in 2017, Burkina Faso is one of the 10 malaria-ridden countries that is not on track to meet targets for disease control mandated by the World Health Organization, according to the study. In many ways, it was the obvious place to erect the MosquitoSphere, according to Brian Lovett, an entomologist at the University of Maryland and the study’s lead author.

Soumousso has been a hotbed of malaria research since the 1980s. The village hosted out some of the first-ever tests of insecticide-treated bed nets, according to Science. At first, it seemed like these nets were a magic bullet. They saved millions of lives by combining traditional physical protection from mosquitoes with pyrethroid insecticides, which generally pose little threat to mammals and are highly effective against bugs in low doses. Invariably, however, mosquitoes find a way to out-evolve our best efforts to contain them. They grew resistant to the insecticide, and the epidemic raged on. But this history of fighting mosquitoes in Burkina Faso made it an ideal site for state-of-the-art malaria research labs, according to Raymond St. Leger, an entomologist at the University of Maryland and one of the authors of the study. Soumousso in particular is a great place for this, since it knows its mosquitoes so well: what subspecies are present, how their populations are structured, and which are insecticide-resistant, Lovett says.
These labs, along with others in sub-Saharan Africa, have played with fungus as a possible mosquito exterminator for over a decade. In 2005 scientists experimented with a naturally occurring fungus called Metarhizium, a natural enemy of the mosquito. Its spores did manage to kill malaria-transmitting mosquitoes in a trial in Tanzania, but not fast enough to stop them from transmitting malaria, and some mosquitoes didn’t absorb enough spores to kick the bucket. In years of research, no fungus has emerged that could kill swiftly and effectively enough.
The researchers from Maryland and Bobo-Dioulasso decided to try out a genetically engineered, superpowered strain of Metarhizium that combines the spore-specific delivery of a fungus with the stopping power of another order of creatures entirely. “Spiders have been engineered through evolution to create proteins that specifically kill insects,” Lovett says. “So we’re using the fungus as a way to deliver that toxin into the blood of an insect.”

They chose the Blue Mountains funnel-web spider (Hadronyche versuta), from New South Wales, Australia. The critters pack a lot of punch in their venom, and the toxin in it is one of the few insecticidal proteins deemed safe for use around humans, Lovett says. The venom first must be extracted in a process called milking. Glenn King, a biochemist at the University of Queensland, milked many a funnel-web spider (a tricky process that involves placing the spider in a tiny contraption that massages the muscles around their venom glands so they drip directly into a tiny vial) for the malaria research team.
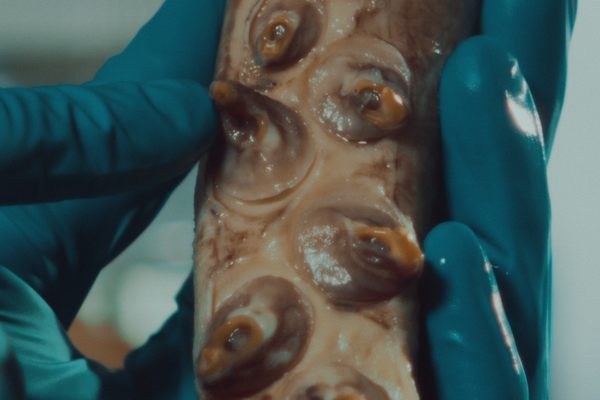
To bioengineer this super-fungus, researchers spliced in a gene that allows the spider to produce its toxin. For good measure, they threw in an extra genetic switch to ensure the fungus only produces the toxin when it comes in contact with a mosquito’s hemolymph (the insect equivalent of blood). Once the venom is in the fungus, the next challenge was to determine where and how to disseminate the spores. The researchers sourced locally available black cotton cloth, soaked it in a solution of sesame oil and spores, and then hung the sheets in the MosquitoSphere.

You may be wondering: Why the domes? Why not, perhaps, a controlled laboratory setting with little threat from the rainy season or a coup? According to guidelines from the World Health Organization, findings in lab-bound mosquito research cannot be extrapolated to the unpredictable, complicated world outside. So a net enclosure is the right kind of controlled setting to simulate a natural environment, where mosquitoes ought to behave more or less like they would anywhere else.
Designed by a Finnish architect, the MosquitoSphere resembles three large, connected greenhouses, subdivided into six smaller compartments, all under a roof of double-layered netting. Four of the compartments contain test huts, native plants, and mosquito breeding sites. “It’s a striking sight when you’re driving up alongside the village,” Lovett says. “The netting started out white, but the soil is very red, so now it’s pinkish brown.”
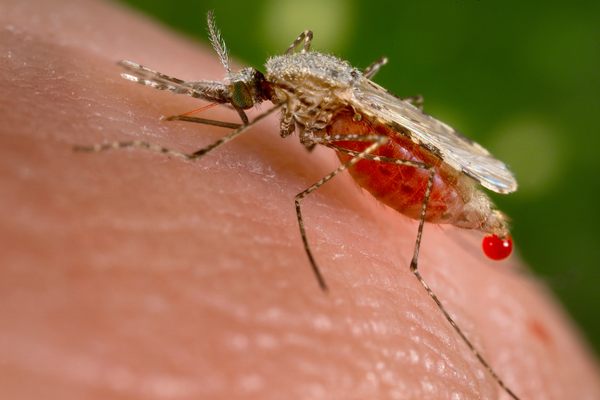
To acquire their tiny, sacrificial test subjects, the research team had locals from Soumousso collect larvae of the insecticide-resistant Anopheles coluzzii mosquitoes from puddles in town. Larvae don’t carry malaria—adult mosquitoes pick it up from biting an infected host—which guaranteed that the experiment would be parasite-free. The researchers reared these grubs into adults within the enclosure.

The scientists’ first stab at the experiment sounds something like a witch’s spell. At twilight, the researchers released 100 female insecticide-resistant mosquitoes into each hut so the insects could feed on the blood of a calf. (The calves are generally undisturbed by this, since they’re not exposed to any more mosquitos in the enclosure than they would be outside.) The bugs were later collected to be monitored for fungal infections. As the work evolved, the researchers hung sesame oil–soaked cloth on the walls of three separate huts, each within its own netted chamber. One piece of cloth was laden with the genetically engineered spores, one with natural spores, and one with no spores at all. The researchers then released 1,000 adult male and 500 adult female mosquitoes into each chamber and monitored them for 45 days. In the spore-less hut, the mosquitoes quickly established a burgeoning society of around 1,400. In the hut with natural spores, 450 survived. In the hut with venomous spores, a mere 13 mosquitoes staggered out.
The MosquitoSphere results, though promising, are preliminary. Deploying the fungus in the real world constitutes releasing a genetically modified species, something that makes many scientists cringe, for good reason. It will require much more testing and many layers of bureaucratic approval, an expensive and time-consuming process. But there’s reason to think it might work. Unlike some other fungal spores, Metarhizium is not airborne; its spores are heavy and sticky. The fungus is also extremely sensitive to light, so it will be difficult for it to spread in some kind of uncontrolled way, should it ever make it outside the dome, by accident or on purpose.

Money and technology conspire to make it difficult to control malaria in sub-Saharan Africa, so the researchers are particularly excited about this project it is relatively lo-fi—just sesame oil, spores, and cloth. From the very beginning of the process, citizens of Soumousso have volunteered to assist, and the scientists have trained them to maintain the enclosure so it will be ready for the next wave of experiments. “It is their sphere,” St. Leger says, adding that scientists in Burkina Faso already have plans to continue using the dome for malaria experimentation.
According to Lovett’s best guess, this technology won’t be ready for practical use for another five to 10 years. “We need to have conversations with regulators on international and local levels, and we have to engage the community to get their permission to use this technology before we try it in the field,” he says. “But it’s a scientific milestone.”




















Follow us on Twitter to get the latest on the world's hidden wonders.
Like us on Facebook to get the latest on the world's hidden wonders.
Follow us on Twitter Like us on Facebook